Pressure sores or pressure ulcers, also known as bedsores, are injuries to the skin and underlying tissues that develop when the same skin area is pressed on or experiences repeated friction over a prolonged period. They usually develop on the part of the body that covers bony areas.
This condition might develop in just a few hours, overnight, or might take days. Though it is very treatable, treatment and care can be costly, especially if the condition recurs or takes a long time to heal. Some bedsores can be life-threatening because they never heal completely.
In this article, Ninkatec Nurses share the essential information about pressure sores, including their causes and risk factors, how to spot a pressure sore promptly, the different means of treating pressure sores, some simple tips on how to care for wounds and ways to prevent them.
Table of Contents
1. Causes of Pressure Sores
A skin area under prolonged pressure receives reduced blood flow, and as a result, a lack of oxygen and nutrients. Over time, this may cause damage to the affected skin and underlying tissues, leading to the formation of wounds. These wounds are called pressure sores or pressure ulcers.
Like other wounds, pressure sores may worsen when bed sheets or clothes rub against them or if patients are handled roughly on the bed or wheelchair. They may become infected by bacteria which in severe cases, may lead to cellulitis (infection of the deeper layer of the skin), osteomyelitis (infection of the bone tissue) and sepsis (a life-threatening situation in which the body’s immune system overreacts to the infection).
2. Risk Factors of Pressure Sores
People who have medical conditions that hamper their normal movement are at the highest risk of developing pressure sores. According to a study, more than 50% of wheelchair users develop pressure sore at some point. It is even more prevalent among bedridden people, affecting up to 80% of those who are cared for at home.
Apart from limited mobility, there are several risk factors that may increase the chance of developing a pressure sore:
- Poor nutrition or malnutrition: without sufficient supply of protein and vital nutrients, the body is more prone to injuries and has a harder time to heal wounds. For this reason, caregivers of frail elderlies who are chair or bed bound should pay special attention to preventing pressure sore.
- Having bowel or urinary incontinence: urine and feces may further irritate the affected skin.
- Excessive moisture or friction: constant perspiration, rubbing on skin, etc may weaken the skin.
- Impaired sensation, e.g., due to complications of diabetes: patient may not feel pain and sores grow unnoticed until late stage
- Medical conditions that affect blood flow, eg., vascular disease
- Obesity or a chronic condition that weakens the body’s overall immune system
3. Common Areas Where Pressure Sores Develop
Generally, while pressure sores can affect any part of the body, they usually develop on bony body parts, such as the shoulder blades, hips, tailbones, spines, elbows, heels, and ankles.
For people using wheelchairs, the areas that rest on the wheelchair are the most frequently affected. These include buttocks (tailbones), spine, shoulder blades, and the back of the legs and arms.
People who are bed-ridden tend to develop bedsores on areas that are in constant pressured contact with the hard surface of the bed, such as the side or back of the head, heels, ankles, behind the knees, hips and buttocks, and shoulder blades. Patients who lie on the side may even develop sores near the ears.
4. Stages of Pressure Sores and their Symptoms
The majority of pressure sores develop in stages and worsen if the affected areas are not cared for or treated properly. You can almost always ascertain how severe the ulcer is by its signs and symptoms. In a few cases, the injury is deep in the skin or covered by other tissues, making it challenging for the doctor to determine staging.
Here is what to look out for stage by stage for most pressure sores:
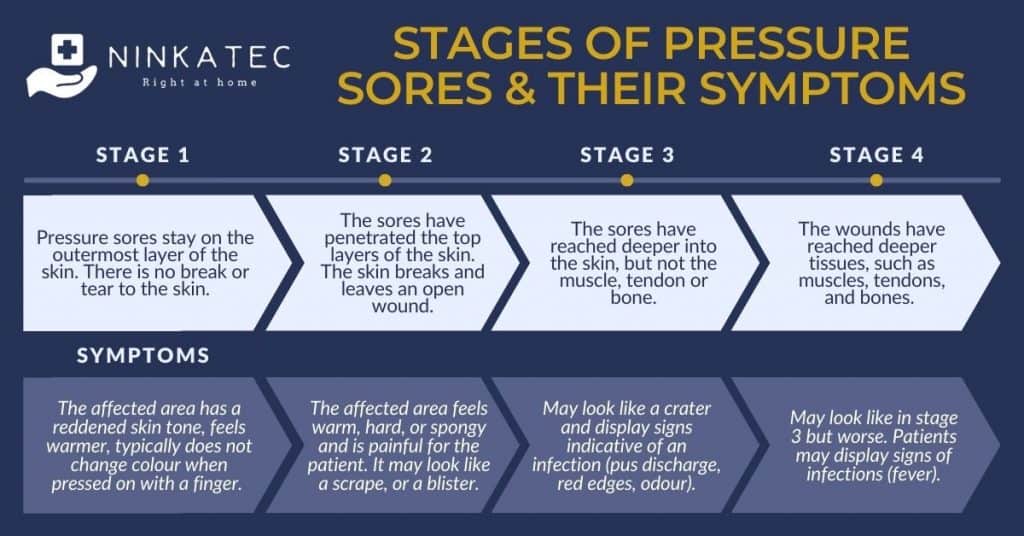
Stage 1:
- In stage one, pressure ulcers stay on the outermost layer of the skin. There is no break or tear to the skin in this mildest stage.
- Signs & symptoms: The affected area has a reddened skin tone. In people with dark skin, this may appear as purple or blue blotches. Skin does not lose its color (i.e., become lighter in color) when you press your finger on it. Skin temperature is usually warmer and can either feel firmer or softer than the surrounding areas.
Stage 2:
- In stage two, the ulcers have penetrated the top layers of the skin. As a result, the skin breaks open and leaves an open wound.
- Signs and symptoms: The affected area feels warm, hard, or spongy and is painful for the patient. You may see a scrape, or a blister with or without clear fluid.
Stage 3:
- At this stage, the pressure sores have gone deeper, reaching the fat tissues beneath the skin, but not the muscle, tendon, ligament or bone. The wound may somewhat resemble a small crater.
- Signs and symptoms: A stage 3 pressure sore may display signs indicative of an infection. These include pus discharge, red edges, odour. The area around the crater often feels warm to touch.
Stage 4:
- In this advanced stage, the wound reaches deeper tissues, such as muscles, tendons, and bones. Though serious, it may no longer feel painful due to extensive nerve damage.
- Signs and symptoms: A stage 4 pressure sore may look like a bad open wound, e.g., exposed tissues or bones, strong odour, swelling around the wound. Patients may also display symptoms of infections and complications, such as fever.
5. Treatment and Care of Pressure Sores
Stages 1 and 2 sores can heal better if cared for and treated properly. Here are some home care tips that caregivers can use to promote the healing of pressure sores:
- Use air or water mattresses and cushions to relieve pressure may be helpful because it allows smoother blood flow. Avoid using donut-shaped cushions as it adds more pressure on the surrounding areas and reduces blood flow to the affected area. You may want to consult your doctor on the types of mattress and cushions that will be best suited for the patient’s condition.
- Change positions frequently is highly beneficial to relieve pressure on affected areas. A timetable or reminders to keep track of when to change position might be helpful for the patient and/or the caregiver. Patients using wheelchairs are recommended to change positions every 15 minutes. Bed-ridden patients should move about every 2 hours.
- Care for the affected skin regularly: The skin should be kept clean and dry after a bath. Use recommended lotions or ointment to moisturise the affected skin. Take note that pressure sores should not be massaged as rubbing on them will encourage the skin to break down further. If open, wound sores should be cleansed with saline water and covered with a sterile dressing.
Stages 3 and 4 sores can be more complicated in terms of treatment and recovery for the patient. It may take a prolonged time to heal as they have affected deeper layers of tissue. The recovery time for such stages usually range from months to even years before a patient is expected to make a full recovery. Some treatment and care plans may include:
- Regular wound dressing
- Specific procedures to remove damaged tissue
- Prescription of antibiotics to treat infection when necessary
- Periodic follow-up by professionals such as a nurse or a doctor to ensure sores are not deteriorating or causing other complications.
6. Preventing Pressure Sores
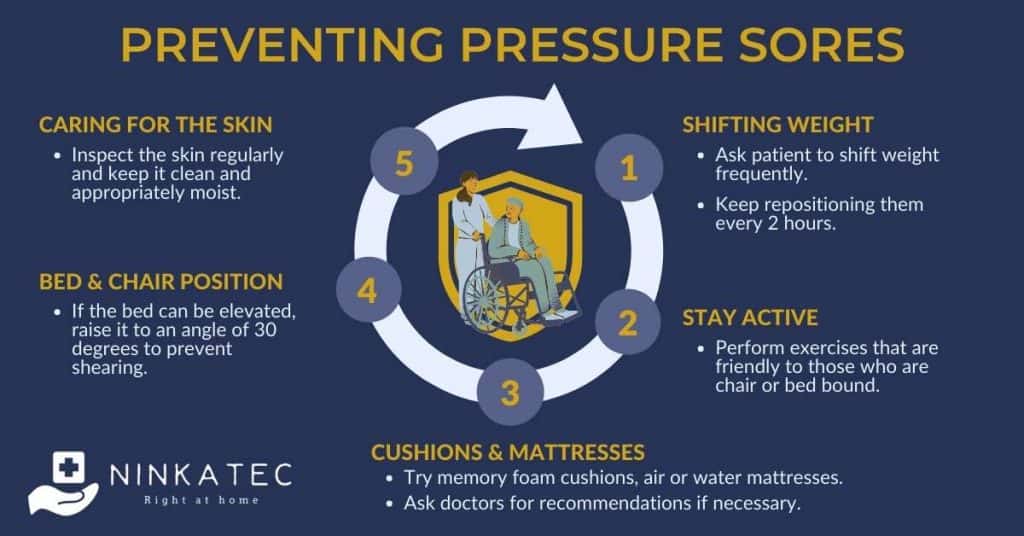
Pressure sores are very common among those with restricted mobility, but they can be prevented. Here are some useful tips.
Frequently shift the person’s weight. If they are bed-ridden or spend most of their time in a wheelchair, as the caregiver, keep repositioning them hourly.
- If possible, encourage and assist the patient with lifting themselves as much as possible. This depends on their body strength. If they are able to lift themselves, try engaging in exercises that are friendly for wheelchair users or bed-bound patients. However, a caregiver or family member should stay close by while the patient is doing this. They can also acquire a specialty wheelchair that allows them to tilt a bit to relieve pressure.
- Use cushions and mattresses that help to relieve pressure and keep the body well-positioned. Some examples can be memory foam cushions, air mattresses or even water mattresses.
- Experiment to find the most comfortable position of the bed or wheelchair. For example, if the bed can be elevated, raise it to an angle of 30 degrees to prevent shearing.
- Inspect the skin regularly and keep it clean and appropriately moist. Pat dry the skin after cleaning or bathing.
7. When to Call for Medical Help
If you care for someone who is bound in a bed or chair for prolonged periods of time, beware that it is quite common to develop pressure sores. It is important to keep yourself informed about the signs and symptoms of bed sores before it happens. When you start noticing any symptoms that develop in your loved ones under your care, keep a close watch. Try to change their position and practise appropriate home care measures but be sure to keep a doctor informed as soon as you can.
If the symptoms worsen and they start experiencing a fever, a draining and smelly sore, increased redness or swelling, seek medical help immediately. Stages 3 and 4 pressure ulcers are to be treated as medical emergencies.
8. Get professional care for a pressure sore at home with Ninkatec
Ninkatec brings nursing care to your doorstep for the comfort of your loved one. Our team of compassionate and experienced nurses conduct home visits to care for our patients who needs a wide range of nursing procedures at home, including:
- Feeding tube procedures
- Urinary catheter procedures
- Home IV treatment
- Injection at home
- Blood-taking at home
- Vaccination at home
- Other nursing procedures at home
We also offer extensive caregiver's guides to NG tube care, urinary catheter care, wound care, stoma care, and care for bed-ridden patients at home on our blog. Check them out and contact us via email, call, chat or web form when you need support with nursing procedures at home.