With age comes the wisdom we are proud of, but also problems such as the loss of muscle and bone mass. Weaker muscle may result in a medical condition called sarcopenia, while weaker bones may develop into osteopenia, and then osteoporosis. The danger is that these silent diseases often do not manifest in ways that prompt seniors to visit a doctor for diagnosis and treatment, until a complication such as a serious fall happens.
Sarcopenia, or age-related muscle loss, has been covered in depth in a separate article on our blog. In this article, we discuss osteopenia and all the essentials you need to know about the elderly’s bone health. Read on to know the causes of osteopenia, symptoms, differences with osteoporosis, the best treatment and preventive measures.
Table of Contents
1. What is Osteopenia?
Osteopenia is a bone-related condition in which bones progressively lose their strength due to the loss of calcium and other minerals, putting a person at increased risk of bone fractures. The condition is more common after the age of 50 - when most people start losing bone density naturally due to aging. It is also more common in women than men. Osteopenia is estimated to affect one in two women and one in four men above the age of 50 in Singapore.
A screening test called bone mineral density (BMD) test measures how much minerals are in our bones and helps the doctor diagnose whether a person has osteopenia. Normal healthy bones have BMD scores ranging between +1.0 and -1.0. Bone mineral density (BMD) ranging between -1 and -2.5 is known as osteopenia and bone density score lower than -2.5 is medically diagnosed as osteoporosis.
2. Osteopenia vs. Osteoporosis
The two conditions are related but not the same. Osteopenia happens when bone density is lower than normal, but not low enough to be diagnosed as osteoporosis. Simply put, osteopenia is the midpoint between healthy bones and osteoporosis. A person with osteoporosis has gone through osteopenia. However, not everyone with osteopenia will develop osteoporosis.
Osteoporosis is considered more severe than osteopenia with a higher risk of bone weakening and fractures. The loss of bone density in osteoporosis is characterised by abnormal holes and spaces inside the bone. These porous or spongy bones can easily fracture or break. In advanced cases, mild pressure when bending over or even coughing can cause fracture. Read more about osteoporosis in our article about common joint and bone conditions here. In this article, we focus on osteopenia, a less severe but also less diagnosed bone disease.
3. Causes & Risk Factors of Osteopenia In Elderly
Aging is one of the most frequent causes of development of osteopenia in the elderly, in both men and women. Bone cells renew throughout our life. However, when a person enters their 50s, the body breaks down bone cells at a faster rate than it builds new bone cells. This leads to the loss of bone density. Bone loss is a part of natural aging, but osteopenia only happens if bone deterioration is progressive and happens faster than the normal speed.
Women are typically at higher risk of osteopenia than men, due to decreased levels of estrogen after menopause - an important hormone in promoting bone cell production in the body. They also absorb less calcium and have lower bone mass than men. There are twice as many women affected by osteopenia as compared to men in Singapore.
In addition to age and gender, other non-modifiable risk factors include:
- Race: The risk of developing osteopenia increases in people of Asian descent and Caucasians.
- Chronic Inflammation: Certain inflammatory diseases, such as Crohn’s disease and rheumatoid arthritis also increase likelihood of developing osteopenia.
- Family history: Seniors with a family history of osteoporosis and early bone loss are more likely to develop osteopenia.
Lifestyle factors can also contribute to or accelerate the decline of bone mass in older adults, including:
- Lack of physical activity
- Lack of exposure to sunlight
- Certain medications, such as some anti-inflammatory drugs have been linked to osteopenia
- Vitamin D and calcium deficiency
- An eating disorder or poor diet habits that results in insufficient supply of vitamin D and calcium
- Excessive consumption of soda and carbonated drinks has shown to increase the risk of osteopenia and osteoporosis among the elderly
- Excessive alcohol consumption
The good news is that lifestyle changes can prevent these causes and lower the risk of osteopenia among seniors.
4. Symptoms Of Osteopenia
Osteopenia has no apparent symptoms, giving it the name of a silent disease. The condition may be present for many years without being diagnosed. In many cases, osteopenia is only diagnosed when a person visits a doctor to treat a bone fracture or a pain in the affected bone. At this point, a bone density test is conducted, often to confirm the presence of osteopenia, or worse, osteoporosis.
If you or your elderly loved one identify with any of the risk factors of osteopenia above, it is recommended to have a discussion with your GP and request for a referral to take the bone mineral density (BMD) scan to check your bone health. According to the National Osteoporosis Foundation, you are a candidate to get your BMD tested if you are:
- Postmenopausal
- A woman aged over 65 years.
- A man over 50 years with one or more risk factors.
- Have broken a bone after age 50.
- A postmenopausal woman with a high chance of breaking bones.
- Have had surgery to remove ovaries
The BMD screening is a relatively quick, non-invasive and painless test. It lets you know the status of your bone health so you can take appropriate actions to preserve it.
5. Complications Of Osteopenia
Since osteopenia predisposes osteoporosis, the most common consequence is osteopenia. If not treated early, osteopenia can progress to osteoporosis which has many complications, including stooped fracture, bone fractures, severe pain, and inability to walk or engage in activities of daily life (ADL). When fractures occur, they take more time to heal with age.
Research has also pointed out a relationship between osteopenia/osteoporosis and sarcopenia. Elderlies suffering from both muscle and bone loss are often seen to be at high risk of frailty and losing their independence in daily activities.
It is important to get an early diagnosis for osteopenia and manage the condition before it gets worse. Preventing osteopenia from developing into osteoporosis requires lifestyle modifications, healthy diet plans, and exercising regularly, as we will discuss shortly.
6. Diagnosis Of Osteopenia
The most common diagnostic procedure for testing BMD is a Dual-Energy X-ray Absorptiometry (DEXA) Test.
The DEXA test is used to measure bone mineral density in the total body, hip, finger, heel, wrist and spine. The test uses a low radiation x-ray beam to measure the BMD. The results of the DEXA test will give you your T-score, based on which you will know if you have normal BMD, osteopenia or osteoporosis. 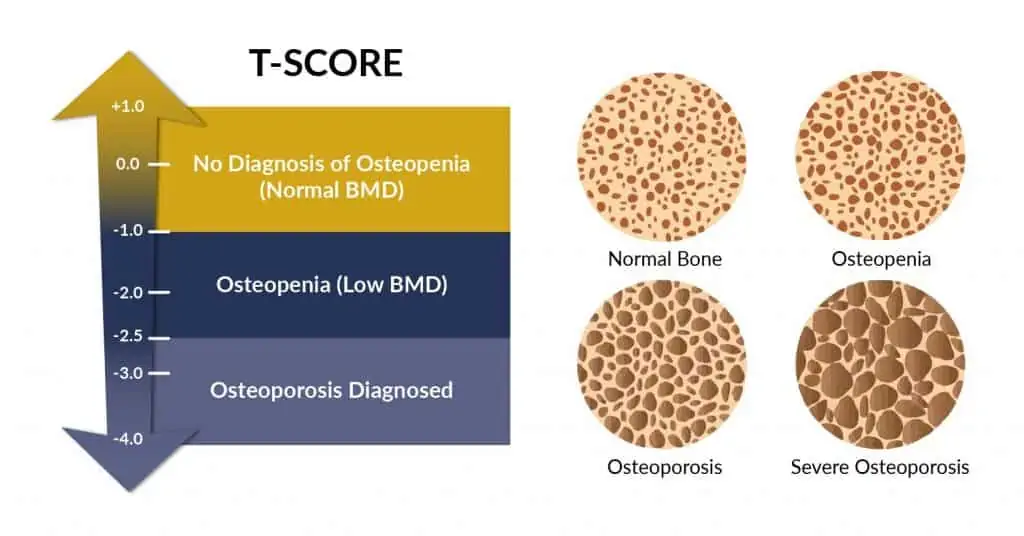
Other diagnostic approaches also used for osteopenia diagnosis include:
- Quantitative ultrasound densitometry (QUS)
- Quantitative computed tomography (QCT)
- Peripheral quantitative computed tomography (pQCT)
- Peripheral dual energy x-ray absorptiometry (pDEXA)
7. Treatment For Osteopenia
Proper treatment is important for patients with osteopenia to prevent it from developing into osteoporosis. Doctors typically do not prescribe any medication during the early stages when osteopenia has a lower risk of bone fractures. Medications are more frequently prescribed when a patient’s BMD level is close to that of osteoporosis.
The early treatment intervention therefore involves mostly lifestyle modification and healthy dietary habits. Let us look at diet and exercise options for people with osteopenia in the following section.
Diet for Osteopenia
Eating foods rich in vitamin D and calcium can help people with osteopenia strengthen their bones. If you do not have osteopenia, sufficient dietary intake of vitamin D and calcium can help you keep the condition at bay.
To ensure a healthy supply of calcium, consume foods rich in calcium, such as:
- Wild freshwater salmon
- Spinach
- Broccoli
- Dried beans
- Dairy products, including yogurt, milk, cheese.
- Sardines
Rich food sources of vitamin D include:
- Fortified cereals
- Orange juice
- Mackerel
- Oily or fatty fish
- Beef liver
Calcium and vitamin D supplements may be prescribed by your doctor if dietary intake is not enough. The daily recommendations on vitamin D and calcium intake by age groups are:
Calcium:
- 1000 mg daily for young men and women.
- 1200 mg of calcium, including calcium supplements and diet, for women of over 50 years entering menopause and men of 71 years old.
Vitamin D:
- 400 IU of vitamin D for infants of 6 months old.
- 600 IU of vitamin D for children, men, and women.
- 800 IU of vitamin D for men and women aged over 71 years.
As you can see, contrary to popular belief, our bodies need more, not less, calcium and vitamin D as we age. Seniors tend to eat less, which reduces overall intake of these nutrients. It is therefore crucial to boost appetite and ensure a healthy diet regime that provides sufficient calcium and vitamin D for our elderly loved ones. We published a guide to proper nutrition in golden years that can be useful for caregivers and seniors here.
Exercises for Osteopenia
Exercising regularly not only treats osteopenia, but also prevents its progression to osteoporosis. Exercises, especially weight-bearing exercises are proven to help prevent further bone loss, build bone mass and reduce the chances of falling.
You can strengthen your bones with moderate-intensity aerobic exercises such as cycling, running, or brisk walking, for 30 minutes a day, 5 times a week, or a total of 150 minutes a week. Yoga, tai chi, and other weight-bearing exercises, including stair climbing or dancing are other good ways to promote bone strength among the elderly.
Exercises with weight, also called strength training or resistance training, should also be incorporated as a part of the exercise regime to improve bone strength for osteopenia patients. Example exercises include:
- Using weight machines
- Weight lifting
- Body weight exercises, like squats and push-ups.
Aim to exercise outdoors as much as possible. Exposure to nature's “sunlight vitamin” helps the body absorb calcium more efficiently.
Though the risk of fracture is low among people with osteopenia, it is essential to always ensure safety and avoid falls, accidents or overtraining during training. Fracture and injury often takes longer to heal for elderlies affected by osteopenia. Learn how to keep your home senior-safe and make exercises comfortable for your elderly from our blog post '8 ways to provide better home care for your elderly loved one'.
Medications for Osteopenia
Besides over-the-counter vitamin D and calcium supplements, your doctor may also prescribe medications to patients in advanced stages of osteopenia to avoid any complications, including permanent bone mass loss.
8. Preventing Osteopenia
The best way to prevent osteopenia is modifying lifestyle habits, dietary habits, and engaging in physical activities. The following preventive tips to reduce the progression of osteopenia are useful for everyone, not just seniors who are at risk of osteopenia. For younger readers, you do not need to wait until you enter your 50s to start a lifestyle that promotes bone health. It is never too early to invest in our bone health.
- Eating a balanced and healthy diet.
- Getting regular exercise.
- Avoiding tobacco exposure.
- Quitting smoking.
- Limiting alcohol use.
- Getting vitamin D and calcium through diet and supplements.
- Getting small amounts of vitamin D from sun exposure.
9. Takeaway Message
Osteopenia is a disease with high burden for individuals, their families and the society, with its high costs for treatment at late stage, the risk of disability and life dependency. Although osteopenia affects half of the female population and a quarter of the male population of 50 years old and above in Singapore, its silent nature makes many people unaware of their condition.
Fortunately, the tools to check one’s bone health and reduce the risk of osteopenia are all within our reach. You are recommended to go for Bone Mineral Density screening if you have one or more osteopenia risk factors mentioned above. If you are diagnosed with osteopenia, you can stop and slow down its progression by eating a balanced diet rich in vitamin D and calcium, exercising regularly, and taking vitamin D and calcium supplements. Our quality of life in the golden years can be made more fulfilling with a healthier lifestyle and stronger bones.









