Headaches are very common. Almost every adult has experienced it at some point in life. But when headache recurs or doesn’t go away quickly, it can be frustrating, debilitating, and costly to individuals. According to a local study, just migraines alone costs Singapore a staggering amount of over $1 billion a year in healthcare costs and productivity loss.
In this article, we discuss what causes the head to hurt, the different types of headaches, and where and how to get treatment. Read on to learn how to self-manage the headaches at home, when to see a doctor, and when a headache could be indicative of a serious issue such as a stroke. We will also cover ways to prevent headache and migraine triggers and improve your quality of life.
Table of Contents
1. What Causes a Headache?
A headache refers to the sensation of pain in the area of the head. It occurs when specific nerves in the body react to triggers, sending pain signals to the brain. It is important to note that the triggers can be related or unrelated to the head and the brain. For instance, a strong smell or certain ingredients in the food you eat can precipitate a headache. Many people can relate to having a headache after waking up from a restless night, or even a day nap. A viral infection can also manifest with a headache, among other symptoms.
Headaches have various possible causes, including:
- An issue in the head and neck area – Such as sinusitis, tonsillitis, toothache, eye problem, ear infection, neck strain, TMJ disorder (TMJ is the joint connecting the jaw and the skull). Management of headache in these cases requires identifying and treating the underlying cause.
- An infection in the body – Headache is a commonly reported symptom of common cold and flu.
- Hormonal fluctuation – Some women experience hormone headache during menstruation or menopause, which is believed to be due to the drop of oestrogen.
- Medication – Referred to as medication overuse headache (MOH), this type of headache most often happens to people over-relying on painkillers to relieve their headache. They feel temporarily soothed, but the headache recurs because the triggers are unmanaged. Over time, this becomes a cycle of needing more medications to get relief from more frequent and/or more severe headaches.
- Lifestyle causes – You may experience a headache due to stress, having a restless night, skipping a meal, not drinking enough water (known as dehydration headache), exercising too vigorously (known as exertional headache), or even not exercising enough. This type of headache typically goes away with adequate rest, and proper hydration and diet.
- Food – Alcohol, caffeine and MSG are known headache triggers. Foods high in nitrate and tyramine such as smoked, cured and processed meat are also reported to be risk factors of headache for some people.
- An issue related to the brain itself – Although this is the most feared problem when someone has a lasting or severe headache, it is very rare. In the event this is indeed the cause, it might be a case of meningitis (infection of the brain or spinal cord membranes), encephalitis (infection of the brain itself), stroke, an injury in the brain, or a brain tumour. We will discuss how to identify the signs and get urgent medical care in the next part.
2. Prevalence of Headache
Headache affects people of all ages, including children. Women are affected by headaches more than men. The diverse causes of headache we discussed above explains its prevalence. Among adults, half of the people aged between 18 and 65 globally are reported to have had a headache at least once in the last year, according to WHO. However, many suffer in silence, self-medicate and do not seek professional care.
Reasons for not seeking medical care vary. For many people, headaches come and go and are often manageable with pain relievers. Others resort to self-treating because they are unaware that effective treatment exists or unsure which doctor to go to.
General practitioners are your first line of care for headaches, except for in emergency cases. Self-treatment without a definitive diagnosis is not advisable. It may exacerbate the situation, leave the underlying causes unmanaged, or lead to medication overuse.
3. When A Headache is An Emergency
Seek immediate care if you experience severe headaches accompanied by one of more of the following symptoms:
- Persistent high fever.
- Difficulty breathing.
- Excessive vomiting.
- Stiff neck.
- A sudden rash.
- Blood pressure of 180/120 or higher.
- Confusion or disorientation.
- Paralysis.
- Seizure.
- Severe eye pain – This could indicate an acute angle closure glaucoma (AACG) which can result in blindness without timely intervention. Contact an ophthalmologist (eye doctor) or emergency service immediately.
- Slurred speech, blurry vision or weakness on one side of the body – These can be symptoms of a stroke. Use the BEFAST method to check for the possibility of a stroke and head down to the A&E department urgently if you recognise the signs.
A particular type of headache called thunderclap headache also needs urgent attention. It may or may not come with any other symptoms. Like its name describes, it feels like a sudden excruciating pain, often peaks quickly and does not last long. Contact your healthcare provider immediately for advice.
4. When to See a GP Doctor for Headaches
Occasional headaches that go away with rest, hydration and nutrition do not need to be checked by a doctor. Excluding the urgent scenarios described above, it is advisable to seek the opinion of your GP or family physician in the following situations:
- Your headache worsens over time.
- The headache does not improve with the appropriate dosage of non-prescription painkillers.
- Headache that makes you take painkillers for 2 weeks in a row.
- Headache that interferes with your work, study and daily activities.
Adults over the age of 50 who develop a new or progressive type of headache should have it checked as soon as possible. It could indicate more serious underlying issues compared to headache in younger individuals.
5. Diagnosis of Headache
When you see a GP or family doctor for a headache, diagnosis will follow a step-by-step approach. The doctor will first conduct an examination and ask you about the history of your headache and other medical details, if they do not have a record. The purpose is to rule out any ‘red flag symptoms’ that necessitate urgent treatment, such as a stroke or a brain infection, or referral to a specialist, such as to an ENT doctor for sinusitis or a dentist for TMJ.
Once these causes are excluded, the condition is categorised as a primary headache disorder, which is to say it has no other causes other than the headache itself. Primary causes account for over 90% of patients visiting a doctor for headaches.
There are 3 main types of primary headache, and part of the diagnosis is to find out what type of headache disorder you may have. The 3 types are:
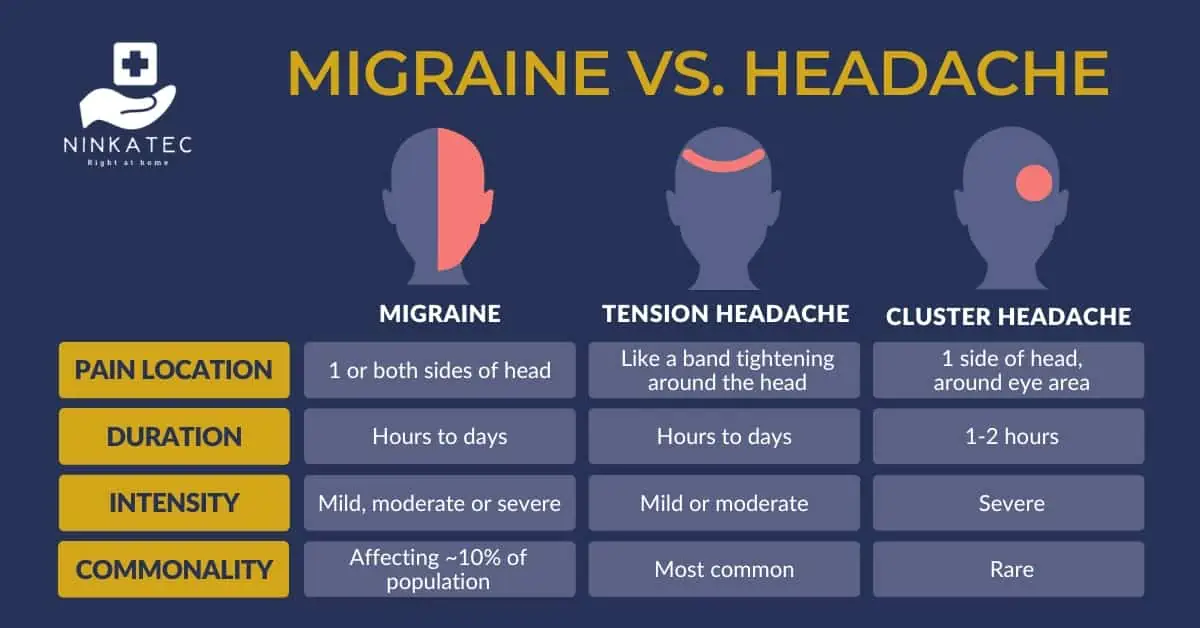
- Tension type headache – The most common type of headache, often feels like a band tightening around the head.
- Migraine – Affecting approximately 10% of people worldwide, 3 times more women than men, migraine causes a variety of symptoms, including a pulsating headache usually on one side of the head.
- Cluster headache – This type of headache is relatively rare, affecting men more than women. It is typically described as a sharp pain in one side of the head, around the eye area.
For a quick and accurate diagnosis, it is essential that the patients describe their headache accurately. For instance, a pounding, pulsating or throbbing headache is more likely to be associated with migraine, while a pressing or squeezing headache that feels like a band tightening around the head is more common with tension headache. The location, duration and severity of the pain could also help with diagnosis. Migraine usually affects one side, tension headache affects both sides, and cluster headache usually causes pain around the eye. Presence of other symptoms such as nausea, light sensitivity, seeing halos or sparkles may point to migraine.
The doctor often helps you along by asking detailed questions. It is okay to say you are not sure of the details if that is the case. You may be visiting the doctor when the headache has gone away and have difficulty recalling. But make a point to take note of the characteristics of your symptoms when the headache recurs. They are very helpful for the doctor to make a diagnosis.
6. Treatment of Headache
Treatment of secondary headache (headache with other causes such as sinus or dental issue) focuses on addressing the root cause, while treatment of primary headache disorder focuses on relieving pain and preventing recurrence.
Medications can be prescribed to help you deal with headache attacks, or as a preventive measure, depending on the type of headache disorder diagnosed and its severity. However, pain relievers of any kind, for headache or other types of pain, should be used strictly as prescribed, as overuse can exacerbate the situation. It can even lead to a medication overuse headache.
A crucial part of the treatment plan is identifying headache triggers and avoiding them. While there are common known triggers among people with recurring headaches associated with primary headache disorders, they differ from one individual to another. It is important to know what predisposes your headache attacks and manage them.
Some of the commonly reported triggers include:
- Stress.
- Lack of sleep.
- Irregular meals.
- Insufficient intake of water.
- Overconsumption of caffeine (tea, coffee, cola).
- Foods (wine or other alcohol, processed meat, cheese, etc).
- Menstruation in women.
- Lack of exercise.
- Environmental factors such as weather changes, glaring light, loud noises, strong smell, etc.
Talk to your doctor if you have difficulty identifying your personal triggers. The doctor may be able to help you by suggesting useful tools such as a headache diary or migraine tracker. These tools are used to track not just the headache but also details that can shed light on the patterns of your headache, such as what food and drink you have, the amount of sleep prior to the headache, and other events. Such information is the basis of an effective management strategy.
7. Non-drug Relief for Headache
You are more likely to hear of home remedies like getting a cold shower, drinking ginger tea, getting massage or acupuncture to relieve headaches from your family and friends, rather than from your doctor. Though this is not a standard clinical treatment method, research has found evidence of effectiveness.
Here are some of the common relief therapies for headache:
- Using a cold or hot compress.
- Getting a cold shower.
- Getting a warm or cold drink, depending on what works best for you.
- Relaxation techniques such as breathing exercises, meditation, light stretching or yoga.
- Acupressure and massage therapy – You can learn self massage on your head and neck or at pressure points on your hands and feet, or get a massage from professional practitioners.
- Acupuncture – This traditional Chinese medicine method inserts fine needles into specific points in the body to relieve pain. Always choose a skilled practitioner, as acupuncture involves risks such as infection and injury.
8. Comorbidities of Primary Headache Disorder
Comorbidities refer to health conditions that coexist in one individual. They may or may not have a causal relationship with each other. A recent research found that more than 1 in 2 people with diagnosed primary headache reported having a comorbidity. The conditions include:
- Depression.
- Anxiety.
- Hypertension.
- Back pain.
- Diabetes.
- Ischemic heart disease.
- Stroke.
If you have a primary headache and risk factors for the above conditions, it may be worthwhile to go for screening regularly to keep them in check.
9. Takeaway Message
A headache may be invisible and common, but the impact of frequent headaches can be very real. If you have headaches that compromise your quality of life, know that you do not need to suffer in silence because there are ways to treat them. Learn to recognise the signs of a life threatening headache that need prompt medical care. In the vast majority of other cases, seek care from your GP or family doctor for your headaches. You will be guided to the right specialist, or receive advice on management strategies that help you live a more fulfilling life.
Medication is one of the treatment methods and should not be overused. It is essential to identify your personal triggers and actively avoid them, for lasting improvement. Non-drug remedies may be helpful, select reputable sources and try to see what works for you.