Table of Contents
1. What is Enteral Nutrition?
Enteral nutrition, commonly known as tube feeding, is a method of feeding that delivers liquid nutritional supplements into a person's stomach or intestine. The enteral feeding tube used to deliver the liquid nutrition can also contain medication.
This feeding method is necessary for patients with a functioning gastrointestinal tract but cannot meet their nutritional needs through normal eating. The most common reason is having difficulty chewing due to dental issues, or difficulty swallowing - known as dysphagia. Without the additional nutrition, the patient may suffer from malnutrition or other serious health issues. Tube feeding can be administered temporarily for a period as short as a few days, or permanently for as long as the patient needs.
2. What is Nasogastric Tube (NG Tube) Feeding?
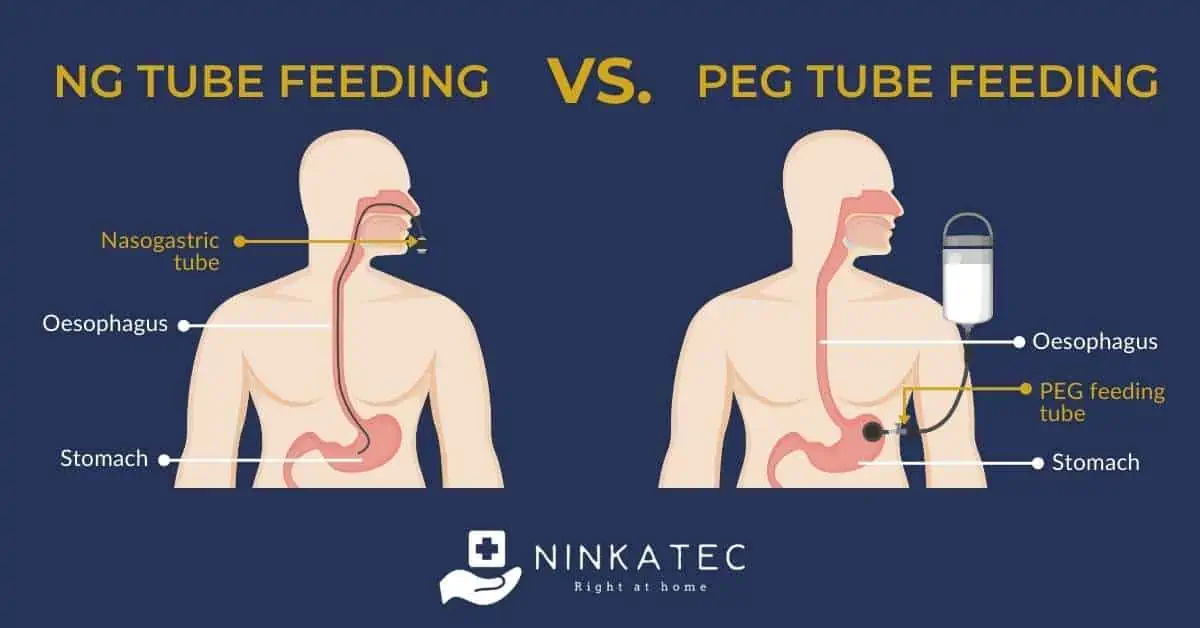
Nasogastric Tube feeding (or NG tube feeding for short) is the most common enteral feeding route used in Singapore. NG Tube is a feeding tube that is inserted through the nose, then through the oesophagus and into the stomach.
Another feeding method used, though much less frequently, is Percutaneous Endoscopic Gastrostomy (PEG). With PEG, the feeding tube is inserted directly into the stomach through the stomach wall.
A survey in 2019 estimated that 97.5% of all patients who need enteral feeding in long term care facilities in Singapore are on an NG tube. Numbers for home care patients are not available but expected to be similar.
3. NG Tube Nursing Procedures by Professional Nurses
The nursing procedures carried out by professional nurses include tube selection, initial insertion, tube stabilisation, replacement and removal. An overview of these procedures are described below, for educational purposes. Patients and caregivers are recommended to check with their own doctors and nurses for specific use and care for their loved ones on NG tube feeding at home.
- Tube Selection:
The tube can be made of PVC, silicone, or polyurethane. They can also have different sizes. A nurse often gives recommendations for tube material and size based on factors such as the tube features, usage duration, the patient's condition and cost effectiveness. The patient and/or family can then decide on the type of NG tube they want to administer.
- Tube Insertion:
Hygiene is of utmost importance in NG tube initialisation. The nurse often performs the procedure in protective equipment (PPE). A typical process involves measuring the insertion length, followed by lubricating the tube, and slowly inserting it through a nostril. Correct placement of the tube is confirmed through a pH test. Once the tube is well positioned, the nurse uses an adhesive to fasten the tube to the patient's nose.
- Tube Changing:
For long term usage, the NG tube needs to be changed regularly. Generally, PVC tubes can be used for up to 2 weeks. Polyurethane tubes can be used for up to 6 weeks (if cared for properly, since they are unaffected by gastric acid). A trained medical professional would assess how often the feeding tube needs to be changed. The caregiver and patient should take extra note to follow the tube changing schedule.
- Tube Removal:
In a tube removal procedure, a towel is often placed on the patient's chest. Any suction used should be removed.. When the tube placement is confirmed, it is flushed with water, then detached from the nose. The nurse pinches or folds the tube and instructs the patient to take a deep breath while gently removing the tube.
4. Responsibilities of Nurses vs Caregivers in NG Tube Feeding
Although certain procedures related to NG tubes are performed by professional nurses, caregivers can learn to administer the daily NG tube feeding at home. Tasks commonly carried out by caregivers often include daily care of the NG tube, administration of feeding, monitoring for signs of tube dislodgement or other complications, and ensuring the tube is changed as required.
5. Home Care for Patients with NG Tube Feeding by Caregivers
For a successful enteral administration, caregivers must follow standard procedures when managing the patient and NG tube. These instructions are provided to the caregiver by the nurse who initialises the NG Tube. Below are a number of important points to keep in mind:
5.1. Preparation of food
Food used for NG Tube feeding is typically of a liquid consistency. The exact food and/or medication and frequency of feeding is determined by the patient's condition. The doctor or dietician will specify what foods to feed or avoid. The patient and family can opt for ready-made liquid formulations or preparing the food themselves. Before feeding, food should be cooled to a temperature comfortable for the patient
5.2. Feeding through NG Tube
Administering feeding through an NG tube may sound complicated but caregivers and family members can learn to perform it successfully with sufficient training and practice. Be sure to feed the patient with the instructed amount and schedule, and follow the steps provided by healthcare professionals:
- Position the patient for feeding
- Check tube placement
- Check gastric content if the patient is ready to be fed
- Use a syringe to pump the food and/or medication through the tube at an appropriate pace
- Flush the tube after feeding with water
5.3. Caring for NG tube
Flushing the tube before and after each feed prevents clogging and infections. After administering medication, an additional flush should also be given to ensure that the full dose is delivered. Warm water can be used for flushing.
5.4. Ensuring the position of tube
An adhesive is usually used to fasten the tube to the patient's nose. This prevents accidental removal or mispositioning. The nasal tape should be changed daily or as and when it loosens.
Patients that require long-term NG tube feeding are usually bed-ridden. Since these patients will be assisted in changing positions frequently, caregivers need to ensure that the tube is not pulled out during this process.
Some patients may accidentally remove the NG tube in their sleep. In such cases, caregivers should never attempt to reinsert the NG tube at home. Instead, consult a doctor for further directions.
5.5. Hygiene and prevention of diarrhoea
Enteral feeding is an ideal environment for bacteria growth. Thus, hygiene is crucial to avoid contamination to the food and infection which could lead to diarrhoea. Caregivers should wash their hands thoroughly before contacting the tube, liquid food, or medication. It is also important to clean the skin around the nose with an aseptic cloth before and after each feed. Caregivers should also wear masks during feeding.
Food should be used quickly after it is prepared. If formula food is prepared, ensure you follow the manufacturer's guidelines. If you prepare your own food, check with a healthcare professional if you are unsure how to handle it.
If you engage a professional caregiver, it is important to specify that you need one experienced in nasogastric tube feeding. Even for professional caregivers, some of them might not receive specific training and have the necessary experience for NG tube handling. Learn more about generalist vs specialised professional caregiver here to engage the best one for your needs.
6. Common Complications in NG Tube Feeding
Complications can arise when caring for an NG Tube at home. Part of the caregiver's responsibility is to look out for complications and ensure tube feeding is comfortable and safe for the patient. Hence, it is important to know what to look out for and how to address issues when they arise, either by yourself or with professional help.
Caregivers are recommended to monitor for the following common complications:
- Tube displacement:
When the tube has been moved from the stomach or intestine, you may see the patient coughing, or bringing up food. These are signs that the tube may be dislodged. Seek immediate medical attention.
- Leakages:
If you see fluid seeping out of the tube, this could indicate leakage. This is likely due to a crack in the tube. In such cases, have a medical professional examine and replace the tube.
- Tube blockages:
A blocked tube means something is stuck inside it, preventing the food from passing into the stomach or intestines. When this happens, you will notice a backflow or very slow passage of food content in the tube during feeding. Seek medical help for this.
- Gastric problems:
Gastric issues could be bloating, constipation, diarrhoea, gas, abdominal pain and vomiting. The bloating could be caused by too much food or air in the tube. This can be addressed with good control of rate, volume, and concentration of feed as well as the provision of fibrous supplements and adequate fluids. In cases of vomiting and diarrhoea, give additional water to the patient to avoid dehydration while monitoring for further development. In some cases, the issue can be resolved by itself. However, if symptoms persist or worsen, contact a healthcare professional.
- Infection:
An infection is a serious complication. This can be caused by prolonged tube use without proper change or a tube blockage. The patient may develop a fever, diarrhoea, mouth sores, etc. Seek prompt medical attention.
- Aspiration:
Aspiration refers to foreign substances such as food, water, saliva moving through the respiratory tract instead of the digestive tract. This is the most severe complication of enteral feeding which, in serious cases, may result in death. You may notice food in the mouth, increased blood pressure or rapid breathing, and wheezing. Sit the patient up and seek immediate medical attention, as this is a medical emergency.
- Skin irritation:
This is primarily caused by the tape used to secure the tube. In some patients, the skin gets damaged and can appear discoloured or appraised. If you notice such signs, try using less tape or ask the doctor or nurse for a more hypoallergenic option.
- Others:
There may be other complications, such as nasal blockage, irritation of the stomach lining, epistaxis, and sinusitis. It is necessary to report to the doctor or nurse any symptom out of the ordinary that you notice, for prompt intervention.
7. Prevention of Complications in NG Tube Feeding at Home
7.1. Oral Care
Patients who receive enteral feeding are at high risk of developing oral infections. They may also experience dry mouth since there is no fluid intake through the mouth. Caregivers should, therefore, assist patients in maintaining good oral hygiene and also help to ease patients' oral dryness using prescribed oral gels or sprays.
7.2. Nose Blockage
Patients with a feeding tube may also experience nose blockage and dryness. Hence, caregivers should check and clean patients' nostrils frequently to make them comfortable. If redness or swelling around the nose is observed, caregivers should seek medical advice.
7.3. Aspiration
To prevent this, caregivers need to pay attention to patients' positioning during and after feeding. The patient's head needs to be kept elevated at 30 to 40 degrees during feeding and should remain in this position for another hour after feeding to minimise the possibility of reflux. In addition, caregivers should also assess tube condition and position while feeding to avoid the formation of boluses (i.e.., food lumps).
7.4. Gastric Issues
Caregivers should also closely monitor patients' bowel movements and functions. Constipation can be prevented by including sufficient fiber in the diet. Gas and bloatedness can be prevented by adjusting the feeding rate and volume, and food content. If possible, encouraging patients to engage in suitable physical exercises may also help with digestion. Check out exercises for patients of different mobility here.
8. When to Seek Medical Help
In addition to changing tubes periodically, professional help is necessary when complications arise. Some situations are emergencies, including:
- If the patient is vomiting
- If patient chokes or have difficulty breathing (signs of aspiration)
- If patient develops fever (signs of infection)
- If the patient is coughing or bringing up food (signs of tube being dislodged - do not reinsert tube on your own)
- If patient experiences persistent stomach issues
- When pH level change
- When the tube has physical signs of getting blocked or displaced
9. Getting Support for NG Tube Care right at Home with Ninkatec
Ninkatec is one of the most trusted home care services in Singapore with an various home care services and plans to suit your needs. Besides NG tube care procedures, we provide a wide range of nursing care procedures at home, including:
- Urinary catheter procedures
- Home IV treatment
- Injection at home
- Blood-taking at home
- Vaccination at home
You can also count on us for:
- House call doctor
- Mental capacity assessment at home
- Being your certificate issuer for Lasting Power of Attorney
- Caregiving (including personal care, companionship and homemaking by professional caregivers)
- Caregiver training
With our team of dedicated doctors, nurses and professional caregivers, we provide both comprehensive long-term care solutions and flexible ad hoc services tailored to your needs. Above all, we maintain an unwavering commitment to quality, compassionate care that honours your loved one's choices and strengthens family bonds during this meaningful time.
Please chat with us or complete the enquiry form below to learn how we can support your family's unique journey.