In our earlier blog post, we discuss the various causes of loss of appetite among the elderly, possible treatments for different causes of poor appetite, what to do at home, when to visit a doctor for treatment, and potential complications if the condition is left untreated. In this article, we dive into the top 4 oral conditions and swallowing issues that can make food and eating less enjoyable for you or your elderly loved ones. The conditions we cover include dry mouth, reduced taste, chewing difficulty and swallowing difficulty.
Understanding these conditions will help you seek the right treatments and identify ways to increase appetite for your elderly loved ones if oral and swallowing problems are the cause.
Table of Contents
1. Dry Mouth
Dry mouth, medically known as xerostomia, occurs when the salivary glands are not producing sufficient amounts of saliva, making your mouth feel constantly dry. Other symptoms may be experienced together with dry mouth, such as bad breath, cracked lips, and dry throat.
Saliva is essential to digest certain food elements. The breakdown of macronutrients starts in your mouth with the help of saliva. This substance also serves as a major defence line to protect your mouth from microbes and maintain good dental hygiene. Dry mouth often leads to loss of appetite. While it is not a serious condition, it does not receive sufficient attention and thus, may remain unmanaged.
1.1. Causes and Risk Factors of Dry Mouth
The prevalence of dry mouth increases with age. However, it is not a natural part of aging. More often, dry mouth happens in older adults because seniors tend to take more of the medications that cause dry mouth. The most common medications causing dry mouth are antihistamines, decongestants, antidepressants, some blood pressure, and heart medications. Some seniors may take these medications daily to manage their chronic condition, and experience long-term dry mouth as a result.
In addition to medications and aging, other causes and risk factors of dry mouth include:
- Stress and anxiety
- Smoking tobacco
- Breathing through your mouth
- Radiation therapy or chemotherapy treatment
- Sjogren’s syndrome - an autoimmune disease that causes systemic symptoms including dry mouth and dry eyes.
1.2. Treatment of Dry Mouth
Dry mouth is typically reversible on its own when you stop using the medications that cause xerostomia or recover from the causes mentioned above. To accelerate the healing process and stimulate appetite, you may also want to employ the following steps to stimulate the secretion of saliva in the mouth:
- Sipping water regularly
- Sucking on ice cubes
- Chewing sugarless gum
- Practise breathing through your nose and using a humidifier at night when you sleep
- Limiting salt intake
- Using toothpaste or mouthwash made for dry mouth
- Avoiding alcohol, caffeine, and tobacco
- Taking saliva substitutes, often available over-the-counter.
1.3. Potential Complications of Dry Mouth
Dry mouth is a benign condition. However, if you develop any of the following signs and symptoms, especially after the primary cause is managed, it is advisable to consult with your primary care physician or dentist for specialised care:
- Altered sense of taste
- Rough tongue
- Cracked lips
- Thick saliva
- Trouble chewing or swallowing
- Bad breath
2. Chewing Difficulty
The jaw tends to shrink as we get older. Together with wear and tear from a lifetime of using the teeth, a smaller jaw makes it more difficult for older individuals to chew foods. Other dental problems such as tooth loss, using poorly fitted dentures, and painful gums add to the chewing difficulty. In some cases, elderlies may find it outright challenging to chew certain foods – a process that eventually may lead to fear of eating and loss of appetite.
According to a study of adults aged 60 and above in Hong Kong, up to 38% of elderlies suffer from chewing difficulties. The same study showed a linkage between chewing difficulty and frailty. Such high prevalence and serious implication convinced researchers to propose chewing difficulties to be included as a geriatric syndrome (i.e., a syndrome of the elderly) and to be screened in primary care.
Chewing difficulty can also have linkage with other diseases, such as neurodegenerative conditions, cognitive impairment or manifest as a symptom of throat cancer.
2.1. Causes and risk factors of chewing difficulty
While difficulty chewing could be the result of several benign conditions, there are some worrisome ailments that precipitate this symptom, such as cancer of the esophagus or throat. Other situations that can also trigger chewing difficulty include:
- Oral mucositis – inflammation of the mucosa, leading to pain, inflammation, and soreness in the mouth.
- Dry mouth – mentioned above
- Dental and gum problems such as loose teeth, tooth decay, tooth loss, gingivitis, and periodontitis. Note that cancer treatment may also trigger gum disease and mucositis, which in turn can result in chewing difficulty.
- Infections of the mouth – caused by bacteria, viruses, or fungi such as oral thrush, hand foot mouth disease, canker sore, oral herpes.
- Pain and stiffness in the jaw muscles – this often occurs when the jaw muscles are overused. Fortunately, the pain is often temporary.
- Radiation therapy on your head or neck – when the radiation beams get in contact with different tissues, you may lose portions of the muscles and bones in your jaw.
- Post-surgical complications – invasive surgeries in the mouth, jaw, or tongue areas may interfere with the chewing process.
2.2. The treatment of chewing difficulty
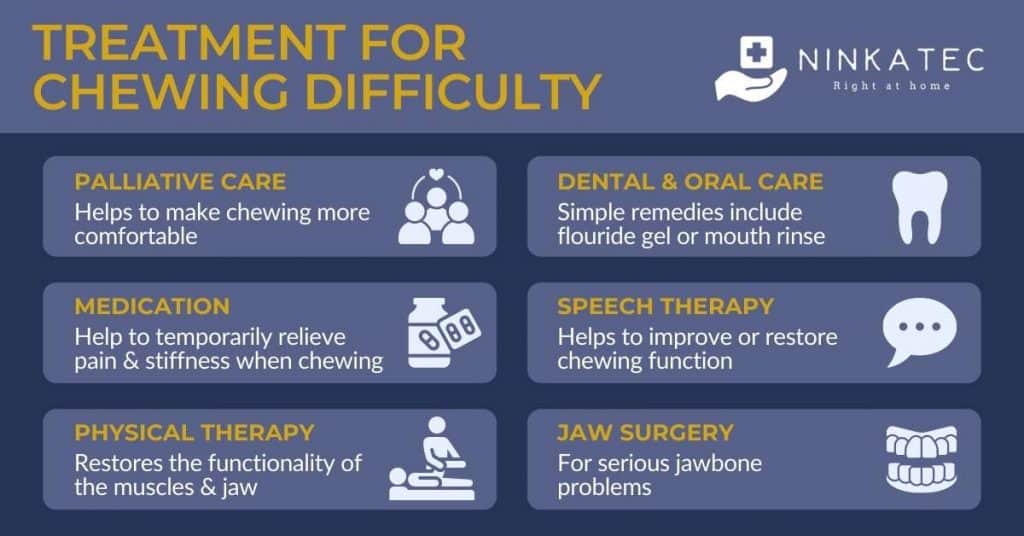
Palliative care – in principle, palliative care aims to relieve the symptoms of chronic illnesses that negatively impact the patient’s quality of life. In the case of chewing difficulty, palliative care helps to make chewing more comfortable and eating more enjoyable (learn more about the benefits of palliative care here). If you are experiencing chewing difficulty due to a chronic disease, speak with your doctor about the best therapeutic approach to address the primary issue.
Dental and oral health care – taking care of your oral hygiene is essential to lower the risk of chewing difficulty. Your dentist will recommend a few oral hygiene routines that improve the bacterial flora in your mouth and the movement of your muscles. If you are taking any medications, especially for cancer treatment, make sure to ask your doctor or dentist about managing the side effects of these drugs that may affect the ability to chew foods. For instance, a fluoride gel or mouth rinse can help prevent this problem.
Medications – if you are experiencing bad pain when chewing food, your doctor may prescribe some painkillers and anti-inflammatory drugs to temporarily relieve the pain and stiffness.
Speech therapy – a speech pathologist can help with issues of chewing after a structural modification of your oral cavity due to surgery.
Physical therapy – physical therapy plays an important role in restoring the functionality of your muscles and jaw after traumatic accidents or surgery.
Jaw surgery – surgery may be a solution to improve jaw strength and chewing ability for individuals with serious jawbone problems.
2.3. Potential complications of chewing difficulty
The primary complication of chewing difficulty is eating less food than you should, which eventually causes nutritional deficiencies. For elderlies, this is associated with frailty, muscle weakness, and compromised immunity. When chewing becomes a chore, it can also make seniors less social, no longer wanting to gather with family and friends over meals, ultimately affecting their quality of life.
3. Reduced Taste
The human tongue has thousands of taste receptors in the taste buds to perceive taste. When food is chewed and mixed with saliva in our mouth, taste receptors detect one of the five basic tastes - sweet, salty, sour, bitter and savoury. The taste buds then send the signals to our brain, telling us how the food we are eating tastes like.
Reduced taste describes a decline in the ability to taste different flavours of food. You may also hear of impaired taste, which refers to an altered sense of taste, such as having a metallic, sour or foul taste in the mouth. Reduced taste sometimes is referred to as loss of taste. However, the complete loss of the taste is very rare. Loss of taste often goes with loss of smell, because taste and smell share some receptors, and they can activate each other. You may notice, food tastes less good when you have a blocked nose.
Elderly adults are known to experience reduced taste as time goes by. According to reports, around 75% of people over the age of 80 have reduced taste.
3.1. Causes and risk factors of reduced taste
In addition to aging as a natural cause, other causes of reduced taste range from completely benign conditions, such as the common cold, to severe conditions which affect the sensory nerves, such as injury in the head or face area, undergoing radiation therapy in the head and neck area, stroke, Alzheimer's or Parkinson disease. Most commonly, it involves conditions in the respiratory system.
Common conditions that affect your ability to taste include:
- The common cold or flu
- Infections of the sinus (sinusitis), throat (e.g., strep throat), or salivary gland
- Gum inflammation, such as gingivitis, periodontal disease
- Medications, such as certain types of antibiotics, antihistamines, antifungal medications or thyroid medications.
- Dry mouth and conditions that cause dry mouth: As you can only taste food that is broken down in liquid, dry mouth prevents you from perceiving the taste of food in your mouth. See previous section for details on dry mouth condition.
- Nutritional deficiencies in vitamin A, B6, B12 or minerals such as zinc and copper.
Smoking is also known to alter the sensitivity of the taste buds, causing a loss of taste or leaving a bitter taste in the mouth when eating food.
3.2. The treatment of reduced taste
The treatment of reduced taste focuses on addressing the underlying condition or cause. For instance, if you have a bacterial infection in your sinuses, throat, or salivary glands, antibiotics prescription will be necessary, after which your sense of taste will return and appetite will increase. Similarly, if it is due to a gum disease, once the dentist has treated it and you start good dental care practice, food will taste better. If you smoke, quitting smoking will help to improve your sense of taste.
If the sole trigger of reduced taste is the aging process, there is little your doctor can do to improve appetite for you. In such cases, addressing other aspects at home to make eating more pleasant, such as making meals more social, mindful eating, or adding spices and herbs to food, may be a good idea. Another tip is to serve warm and hot food, as taste receptors are known to be more sensitive at higher temperatures.
3.3. The complications of reduced taste
Long-term reduced taste can lead to loss of appetite, which in turn can result in malnutrition and frailty. It is therefore important to address the issue early, protecting elderly’s sense of taste as much as possible and preserving the joy of eating for them.
4. Difficulty Swallowing (Dysphagia)
Dysphagia is a medical term that describes persistent difficulty swallowing. Individuals with dysphagia need more effort to move food elements from the mouth to the food pipe. Anyone can experience occasional difficulty swallowing, for example when food is eaten too fast or not chewed well. Such cases are not concerning. However, if difficulty swallowing persists over a period of time, it is important to visit a doctor for an investigation.
4.1. Causes and risk factors of dysphagia
As a general rule of thumb, dysphagia is either the result of a nerve or muscle problem. Underlying conditions and age are two major risk factors. The problem is prevalent among the elderly, estimated to affect 20% of all seniors, and 40% of those who live at nursing homes. Dysphagia is even more common among elderlies with stroke or dementia.
There are 3 types of dysphagia, affecting 3 different phases of the swallowing process:
- Oral dysphagia (also called high dysphagia): Causes are related to problems in the mouth, such as dental issues, jaw or tongue muscle weakness, chewing difficulty, dry mouth or reduced taste as discussed above. Chronic Obstructive Pulmonary Diseases (COPD) and other lung diseases can also cause oral dysphagia, due to difficulty in coordinating breathing and swallowing.
- Pharyngeal dysphagia: The causes of these cases are related to the throat - the second phase of the swallowing process after food is passed from the mouth. This often happens due to neurological damage as a result of stroke, dementia or Parkinson’s disease.
- Esophageal dysphagia (or low dysphagia): Patients having low dysphagia typically report the sensation of food stuck in their oesophagus or chest. Swallowing difficulty of this type often happens due to obstruction in the oesophagus due to a tumor or fibrosis or esophageal inflammation, or damages of the esophagus as a side effect of radiation therapy. It can also be caused by gastroesophageal reflux disease (GERD). In other cases, the muscles of the esophagus do not work well and obstruct food, such as in the case of achalasia - the lower esophageal sphincter is too stiff to allow any food to pass through; or diffuse spasm - muscles of the esophagus contract uncontrollably, obstructing the normal path of food; or esophageal ring - a small portion of the esophagus narrows, acting as an obstacle for solid foods to pass through.
4.2. Symptoms of dysphagia
Dysphagia usually manifests with the following signs and symptoms:
- Feeling of difficulty while swallowing food
- Feeling of having to make multiple swallows for even a small amount of food
- Drooling or leakage of food while eating
- Finding ‘pockets’ of food in the mouth after eating
- Choking or coughing while swallowing food
- Feeling of food stuck in the throat or chest after eating
In cases when dysphagia is caused by GERD, symptoms are similar to those of GERD, including heartburn, the feeling of food regurgitation, or the bitter taste at the back of the throat due to acid and food regurgitation.
In severe cases, patients may experience unintentional weight loss, nutrition deficiency and recurrent episodes of pneumonia.
4.3. Treatment of dysphagia
4.3.1. Treatment for oropharyngeal dysphagia (high dysphagia)
Most cases of oropharyngeal dysphagia are the result of a neurological problem. Therefore, treating this condition can prove to be challenging. Here are some measures that may benefit high dysphagia:
Swallowing therapy — a speech therapist helps individuals with high dysphagia to restore their swallowing reflexes by performing certain exercises that improve the tonicity of the jaw muscles.
Feeding through a tube — if your case of dysphagia is severe enough or other complications arise (e.g., pneumonia, dehydration, malnutrition), placing a nasogastric tube (NG tube) to ensure appropriate feeding may be necessary. In advanced cases, your doctor may recommend percutaneous endoscopic gastrostomy (PEG), which is a tube that gets surgically implanted into the stomach via a small incision in the abdomen.
Diet — focusing on a diet that contains enough nutrients is also vital for recovery from high dysphagia. You see, the condition itself is not life-threatening; however, the malnutrition that arises from it can be very dangerous.
4.3.2. Treatment for esophageal dysphagia (low dysphagia)
Low dysphagia generally occurs when there is a structural abnormality in the esophagus. Here are the available treatment options:
Dilation: if dysphagia results from a stricture, your surgeon may recommend a small balloon to inflate the esophagus.
Botulinum toxin (Botox): Botox is a muscle relaxant that helps the muscles of the esophagus to relax. Most commonly, this medication may be beneficial for patients with achalasia.
4.3.3. Treatment for other cases of dysphagia due to side effect or underlying conditions
When dysphagia happens due to a primary condition such as COPD, treatment focuses on the underlying cause. If the underlying cause has little chance of being reversed such as in the case of advanced dementia or stroke, diet modification such as eating or feeding in smaller bites, changing to pureed type of foods, feeding or eating with cups, straws and spoons instead of bowls could help patients eat better.
4.4. The potential complications of dysphagia
The most common complication of dysphagia is pneumonia and upper respiratory infections. Aspiration pneumonia happens when food content ends up in the wrong ‘pipe’, which is to say it enters the lungs instead of the stomach.
Other complications are similar to conditions discussed above, including malnutrition and dehydration. Malnutrition is especially prevalent in individuals who choose not to treat dysphagia. Over time, the amount and diversity of nutrients sharply decline, leading to malnutrition. Some forms of dysphagia interfere with the ability to swallow fluids, precipitating dehydration.
5. Takeaway message
We hope the article sheds light into the complex process of the seemingly simple act of eating, and possible causes that could make mealtime frustrating for some seniors. Fortunately, for many cases, oral and swallowing issues can be addressed when the underlying causes are identified and treated. Good dental hygiene practice also helps to reverse some of the causes and restore appetite.
Remember that aging brings about subtle changes to the eating habits of older adults. For example, it is common for many seniors to develop a preference for pureed type of food rather than fried and dry food as they get older. In these cases, diet modification works better than medical intervention. Check out our earlier blog post for ideas of food recipes, meal time, meal sizes, and other techniques that can increase appetite and boost nutrition for your elderly loved one.
It is also crucial to ensure adequate nutrition, especially when you have been struggling with appetite and eating. Learn how nutritional needs change with age and what to do to avoid nutritional deficiency as you grow older from our elderly nutrition guide here.