Wound care at home may sound a little scary if you are unfamiliar with it, but it does not have to be. While certain procedures should only be carried out by professionals, most caregivers equipped with basic knowledge of wound care and step-by-step guidance can handle part or all of the wound care processes uneventfully at home.
This article aims to help caregivers with the essentials of wound care at home. We will walk you through what to expect during the healing journey, simple care steps you can safely carry out at home, how to prevent complications and support optimal healing, and signs that you should call for professional help.
Table of Contents
1. What is a Wound?
Any type of injury that causes a break or tear in the surface of the skin is known as a wound. Some wounds are penetrating wounds, which means they break through the layers of the skin as a result of trauma. Others are non-penetrating wounds which do not go through all the layers of the skin.
In a home care setting, a wound may happen as a result of a deep cut, a fall or a burn. Surgical draginage of abscess often leaves a wound that takes time to heal at home. Or if you care for a wheelchair-bound and bed-ridden loved one, they may develop a pressure sore (bed sore) which can progress into an open wound if it is not timely treated.
2. Types of Wounds
It helps to know the types of wounds because treatment and care for each type varies. Medical professionals classify wounds by their severity from Class 1 to 4, with Class 1 wounds being the clean, uninfected and uncontaminated type and the easiest to treat.
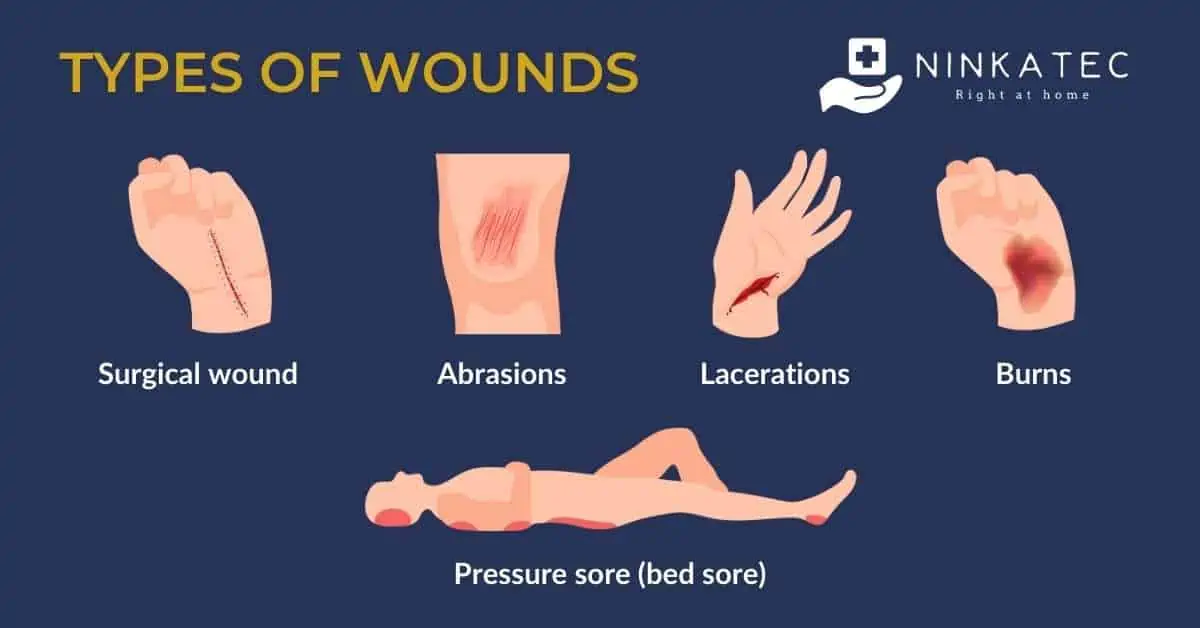
Below are the main types of wounds that a home caregiver may encounter.
2.1. Surgical wound
A surgical wound is a cut made by a surgeon in an operation or a medical procedure. You may hear doctors refer to it as a surgical incision. It can occur anywhere on the body, it may be small or large, depending on the medical issue that requires the surgery. In caring for a surgical wound, it is essential to follow the instructions provided during the hospital discharge and to prevent infection.
2.2. Pressure sore/ulcer
A pressure sore is a small, red area on the skin that can form for even the simplest of reasons, such as if you are wearing heavy shoes or clothing that is too tight. They can also develop when someone lies or sits in one position for too long, which can be quite common among people using wheelchairs or recovering from an illness in bed.
Pressure ulcers form when the pressure on your body is greater than the amount of blood flowing to your skin and tissue, causing the area to swell up. The pressure gradually builds up under the skin and starts to break down the blood vessels, creating blisters. Without timely and appropriate care, they can break down very rapidly and require urgent medical attention.
Since pressure sores are a prevalent issue in home care, we wrote a dedicated article on preventing and caring for it here.
2.3. Abrasions
Abrasions are caused when the top layer of skin is rubbed off, due to friction or injury, such as during a fall when the skin rubs against a hard surface. Abrasions can be very painful, because the protective layer of the skin is damaged or missing. They are quite common in daily life, including among children. An abrasion wound is also known as a scrape or graze.
2.4. Lacerations
Lacerations are caused by deep cuts or tears to the skin, often by sharp and hard objects during a fall, accident, or other blunt traumas. Unlike abrasions, the skin is not scraped off. However, laceration wounds can cut into deeper tissue layers. Minor lacerations which are clean and shallow can be treated at home with antibiotic ointment and bandage. Large lacerations may require stitches (sutures) to heal. Both minor and serious lacerations can cause pain and bleeding.
2.5. Burns
A burn is an injury to the skin or the structures beneath the skin caused by the heat from a fire or heat source. Burns can result from direct contact with flames or high-temperature objects or indirect contact such as burns from hot water or steam. Burn wounds are often classified as first, second, and third-degree burns, and their severity is dependent on how deep they reach into the skin’s layers.
2.6. Others
Other types of wounds include puncture wounds (caused when a sharp and pointed object pierces into the body, such as a nail or needle), diabetic foot ulcers, amputation wounds, bites and stings, etc.
3. The Stages of Wound Healing
Below are the four main stages of wound healing
Stage 1: Stop the bleeding (Hemostasis stage)
When an injury happens, the body detects and attempts to stop the blood loss by itself right away, through a series of processes. One of the main activities is the mobilisation of platelets - the blood cells that can bind together - to form blood clots, which will help build a scab on the surface of the wound. This scab keeps blood in and germs out, allowing the body to heal the tissues underneath.
In certain cases, the natural hemostasis processes might be disrupted, leading to blood loss. Common causes are low platelet count or using blood thinner (i e., anticoagulant) to prevent the risk of a stroke or heart attack.
Stage 2: Repair (Inflammatory stage)
‘Inflammation’ and ‘healing’ may sound like two opposite things, but they both happen to a wound after bleeding has stopped, and for a good reason. Inflammation is actually a natural response to injury. It is believed to promote repair, fighting infection (cleaning) and forming of new tissues.
During this stage, which generally lasts for a few days, you may experience redness, warmth, tenderness, and swelling arounnd the wound. This signals that the body is increasing blood flow to the area to accelerate healing. You may also see clear fluid coming out of the wound. They are signs that the ‘rescue team’ of the body are hard at work.
The challenge for caregivers is to be able to tell from normal swelling and swelling due to infection. We will address it in the ‘Potential Complications’ section below.
Stage 3: Rebuild (Fibroblastic stage)
In this stage, the body activates a number of specialised cell types, including an important cell type called fibroblast to aid with rebuilding the damaged tissues and blood vessels. The fibroblastic stage is also known as the proliferation stage and can last up to a few weeks. The wound starts closing. You may see new skin or a raised reddish-coloured scar forming replacing the brownish-coloured hardened crust on top of the wound. You may also feel itchiness but do refrain from scratching.
Stage 4: Recover (Maturation stage)
Also medically known as remodelling, the maturation stage is when the new cells and tissues regain flexibility and strength. This final stage of wound healing may last for years. During this time, the wound closes completely and the affected area recovers its function. Initial scar tissues are replaced by tissues that look closer to normal skin. For serious injuries or wounds that result in limited range of movement, you may need physiotherapy at this stage to improve functions.
4. Treatment and Care for Wounds
Now that we have an understanding of the different wound types and how they heal, let us discuss how to care for wounds to promote healing.
The first step after a wound happens is to stop the bleeding. The body starts performing hemostasis processes immediately but you can help it out. First aids for stopping a wound bleeding include rinsing the injury area with clean water and applying light pressure over it, using a bandage or clean piece of cloth. Elevating the wound also helps to reduce blood flow to the site.
Note that if you are on blood thinners, the body will have difficulty forming the necessary blood clots. In such cases, you will need to apply pressure for longer, until bleeding stops completely.
The next step is to decide if you can care for the wound at home or need professional care. This depends on the cause and severity of the wound. It is crucial to seek medical care if the injury is deep or big, looks infected or compromised in some way, or if you have a hard time stopping the bleeding, or if there is debris or a foreign object stuck in it. In some cases, wounds look fine and non-infectious but still require treatment because they are painful and cause discomfort for the patient.
Regular wound care you can do at home
If you decide that the wound is safe to be cared for at home, you will need wound care material, including:
- Wound dressings
- Bandages
- A sterile alcohol-free solution or wipe to clean the wound
- A topical antibiotic
- Other tools and materials such as cotton balls, gloves, scissors, protective sheets, etc.
Note that wound dressings and bandages serve different purposes. A wound dressing is a pad or compress applied directly to the wound to protect it, prevent infection and promote healing. A bandage helps to secure the dressing in place. You may see them being combined in self-adhesive form (e.g., plasters).
Below are simple at-home wound care treatments you can carry out:
- Cleaning and drying the wound
- Applying antibiotic ointments to prevent infection
- Bandaging the wound to prevent dehydration
- Using sterile saline packets to soothe the area
One thing that you should note is that home wound care does not mean that you have to do everything yourself. You can also get professional nursing care support when required, but carry out regular wound care by yourself. Be sure to follow the directives provided by the healthcare provider precisely.
5. Wound Dressing at Home
Wound dressing is an essential part of wound care. Its main purposes are to support the Repair stage and part of the Rebuild stage in wound healing, including:
- Protecting the wound and keeping it clean
- Absorbing drainage from the wound and keeping it dry
- Keeping the wound from being dehydrated as moisture helps with healing
Wound dressing often requires daily change for hygiene purposes, or as advised by a healthcare professional. Caregivers should take the chance to observe closely how the wound is healing under the bandage, and seek medical support if something is unusual. Selecting the right type of wound dressing is also important. Certain types of injury may require special dressings, such as in the case of diabetic ulcers. Get professional advice if you are uncertain which dressing type is best for you.
6. Nursing Care Tips to Care for a Wound at Home
It is important for caregivers to understand the basic rules of wound care in order to avoid further complications, even if you have a professional nurse helping with changing dressing and other procedures.
Here are some important points to bear in mind when providing care for superficial, uncomplicated wounds at home:
- Wash your hands before caring for a wound. This helps prevent bacteria from adhering to your skin and transferring to your wound.
- Apply gentle pressure to the injured area with a clean towel or compress until the blood stops flowing. Be careful not to exert too much pressure, as this can increase bleeding.
- Clean the wound thoroughly with clean gauze and sterile saline solution if the area is small enough and easy to reach. If it is a large area that is likely to get dirt in it (like elbows or knees), you should clean the wound with anti-septic solution.
- Ensure the area is always kept clean and dry and discourage removal of the bandage or touching the wound.
- Keep an eye out for complications, such as an infection, excess bleeding, or fever.
- Proper nutrition is another vital part of optimal wound healing. Ensure your loved one has healthy, balanced meals during recovery time.
Certain procedures are best performed by a professional nurse, especially if the injury is complex or if the patient develops complications such as infection or necrosis (dead tissues). We break down the tasks that caregivers generally can do by themselves and those they should rely on medical professionals in the table below.
Wound Care at Home - Responsibilities of Caregiver vs. Professional Nurse
7. Signs that a Wound is Healing Well
A good way to tell whether your wound is healing well is to map it against the expected healing stages. In the first few days, you can look at the extent of the scab. The scab should cover almost all of the wound, leaving only a small hole without a scab over it. The lack of a scab, or a large gap between the scab and the wound could be a sign that healing is disrupted.
Some swelling and inflammation is expected as the body does its repair work. Reasonable pain and discomfort might be part of the experience. When the wound heals well, you should feel better day by day. While some wounds may take longer to heal than others, the lack of progress over time and development of symptoms such as fever, bleeding after the wound has closed, broken stitches, etc. are often signs of complications. We will cover them in detail in the next section.
8. Potential Complications
Complications prolong recovery time, may lead to additional health issues and treatment, affect the patient’s and caregiver’s well-being, and increase medical cost. Thus, preventing complications is crucial during wound care. In this section, we will explore some of the potential problems that may arise and how to deal with them, and best of all, to prevent them from happening in the first place.
8.1. Infection and dehiscence
This is the most common type of wound complications. A simple hand laceration may get infected 5% of the time, according to a study.
An infection occurs when the body fails to fend off bacteria entering the wound, allowing them to grow in it. Dehiscence refers to the opening up at the edge of the wound. Dehiscence can happen due to force exerted to the wound, too tight stitches (sutures) in a surgical wound, or weak muscle or tissues at the wound site. Infection can also cause dehiscence.
Aside from excessive redness and swelling, there are other signs telling you an infection might be going on. You might experience bleeding, pus or liquid coming out of the wound or smell foul odour from it. The patient might develop a fever, feel more pain or discomfort. The injury site may feel hot to touch and more tender and spreading. For dehiscence, you may notice broken sutures, or previously closed wound edges opening. Contact a healthcare provider to get it checked.
To prevent dehiscence, ensure that the patient does not engage in strenuous activity or excess stretching which may impact wound healing . If the patient vomits or coughs a lot and it affects the injury area, use a pillow or soft cushion to limit the impact. Infection can be prevented by ensuring the dressing is done as directed and keeping the wound clean and dry.
Extra caution should be taken for patients with chronic diseases that can weaken their immunity such as diabetes, kidney disease, cardiovascular disease, or those undergoing cancer treatment. They are at higher risk of infection.
8.2. Wound not healing or closing
As discussed above, an injury might look red and swollen during normal healing as it goes through the inflammatory stage. However, if you see the wound not closing well, redness and swelling at the injury site getting worse or taking longer than expected, you should seek medical assistance.
Infection is one of the underlying reasons for delayed healing but it is not always the case. This could also occur because the injury is severe, it is at an awkward angle, the skin around the wound is too thick, or a foreign object is pressing against it. Preventive action is limited in this scenario, but getting professional care promptly will help to ensure the complication does not deteriorate.
8.3. Wound not forming scab
Scab forms the necessary protective layer to cover the injury, for the damaged tissues underneath to be repaired or replaced. This process might be compromised when there is a disruption in blood flow to the site of the injury, leading to slower healing and more pain. This risk increases for people with existing chronic diseases that lead to poor blood circulation, such as diabetes, heart disease and obesity.
To help ensure proper scab formation, you can let your healthcare provider know of your loved one’s comorbidity and ask for advice to improve blood flow to the affected area. Do not attempt to do this without proper directives, as each case is different, and you may end up worsening the condition of the wound.
8.4. Bleeding
Bleeding may happen in the later stage of healing due to known causes such as picking of the wound or new injury. In other cases, if you notice a lot of bleeding that saturates the dressing in a few hours or less, or bleeding that gets worse day by day, it is a cause for concern.
To prevent bleeding, ensure your loved one does not pick on the wound or dressing and no pressure is placed on the affected area. Call for a healthcare professional immediately otherwise, especially if you cannot successfully stop the bleeding completely by yourself at home.
8.5. Necrosis
Wound necrosis refers to dead body tissues that the body can not get rid of at the wound site. It is a serious complication and requires professional removal and handling. It can happen in serious infections, such as with pressure sores (bed sores) in stage 3 or 4, or when blood flow to the injury is severely restricted in some way. People enduring traumatic injury or who are on high-dose corticosteroids are at higher risk of necrosis. The symptoms of necrosis are similar to infection, but often more serious.
Prevent necrosis by attending to pressure sores early, keeping the area clean and. Necrosis may lead to further complications and needs immediate medical attention.
8.6. Pain
Pain is associated with most wounds. It gets better as healing progresses. Ask your doctor for pain relievers if you or a loved one experiences excessive pain. However, if pain is worsening and accompanied by other symptoms described above, it is a sign of complications and you need to contact a medical professional for assessment urgently.
9. When to Call for Medical Assistance
Aside from the above complications, if you are uncertain if you need professional support, always err on the cautious side and contact a healthcare provider in the following scenarios:
- The patient has difficulty walking or moving because of the wound
- The injury bleeds more than usual, compared to the past days or weeks or to what the nurse or doctor has set parameters for you to look out for.
- It looks infected, excessive or prolonged redness, swelling or bleeding
- The wound oozes pus or has a pungent odour
- The patient develops a fever
- One or more stitches are broken
- There is little to no healing after a week or more
10. Takeaway Message
As wound care can be quite involved, the caregiver’s instinct is to help your loved one by either relying completely on a professional nurse or interfering immediately when you see signs of suffering. However, an optimal way is to work together with the medical professional to promote healing throughout the journey. A hands-on wound care training with a professional can give you confidence if you are unfamiliar with the procedures.
Getting Nursing Care Procedures in the Comfort of Your Home with Ninkatec
As one of the leading home care providers in Singapore, Ninkatec enables family caregivers to care for your loved ones right in the comfort of your home. We believe growing old in the loving care of one's family contributes significantly to the senior's well-being in their golden years.
Our team of compassionate and experienced doctors, nurses and caregivers conduct home visits to care for our patients who needs a wide range of home care services, from house call doctors, mental capacity assessment, nursing procedures and caregiving to structured specialsed home care plans.
Our nursing care services at home include:
- Feeding tube procedures
- Urinary catheter procedures
- Home IV treatment
- Injection at home
- Blood-taking at home
- Vaccination at home
- Other nursing procedures at home
We also offer free resources for caregivers including bedsore care and prevention, NG tube care, urinary catheter care, care for bed-ridden patients at home in our series of caregiver’s guides on our blog.
You can also chat with us below if you have any specific questions about wound care or nursing care at home. We are only a text message, call or email away.